WEDNESDAY, Oct. 15, 2014 (HealthDay News) — People with more severe cases of psoriasis may be at increased risk of uncontrolled high blood pressure, a large study finds.
Researchers looking at over 13,000 adults in the United Kingdom found that those with severe psoriasis were 48 percent more likely to have poorly controlled blood pressure, versus people without the skin condition.
The findings, reported online Oct. 15 in the journal JAMA Dermatology, confirm an association between psoriasis and cardiovascular health. But the precise reasons are not clear, and a cause-and-effect link was not proven.
“We still don’t fully understand why we see a higher prevalence of cardiovascular risk factors in people with psoriasis,” said study leader Dr. Junko Takeshita, a clinical instructor of dermatology at the University of Pennsylvania in Philadelphia.
But, Takeshita said, chronic inflammation could be a common denominator.
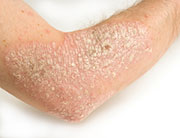
People with psoriasis develop thick, scaly patches on their skin that are often itchy or sore. Experts believe the problem arises from an abnormal immune system attack on healthy skin cells — a reaction that causes chronic inflammation. Chronic inflammation in the blood vessels is thought to contribute to high blood pressure (“hypertension”), heart disease and stroke.
“We’ve known for some time that there’s an increased prevalence of high blood pressure, diabetes, heart disease and stroke in people with psoriasis,” said Dr. Jerry Bagel, a member of the National Psoriasis Foundation medical board and director of the Psoriasis Treatment Center of Central New Jersey.
But this study shows that even among people who are seeing their doctors and have been diagnosed with high blood pressure, those with psoriasis are less likely to have those numbers under control, said Bagel, who was not involved in the study.
“It’s important for primary care doctors to be aware that patients with psoriasis are at risk of uncontrolled hypertension,” Bagel said.
The same goes for people with the skin condition, he added. “Psoriasis is not just skin deep. It comes with metabolic and cardiovascular risk factors.”
But people can make a big difference, Bagel said, through lifestyle choices: eating a healthy diet, getting regular exercise, not smoking and drinking alcohol only in moderation.
The current findings are based on an electronic medical database that included nearly 13,300 adults diagnosed with high blood pressure. Over 1,300 of those people also had psoriasis.
Takeshita’s team found that among people with severe psoriasis — meaning it affected more than 10 percent of their skin — almost 60 percent had uncontrolled high blood pressure (a reading of 140/90 mm Hg or higher).
What’s more, their odds of poorly controlled blood pressure were 48 percent higher, versus people without psoriasis, the study found. Meanwhile, people with moderate psoriasis (at least 3 percent of the skin affected) had a 20 percent higher risk.
The researchers did consider other factors that affect blood pressure control, including people’s weight, smoking and drinking habits, and use of medications that can boost blood pressure. But psoriasis itself was still associated with a higher risk of uncontrolled high blood pressure.
Takeshita agreed that the findings bring more awareness to the cardiovascular risks many people with psoriasis face.
“Even among doctors, there’s still an under-recognition,” she said.
A big question, Takeshita noted, is whether getting severe psoriasis under better control with medication can improve people’s cardiovascular health, too.
“There are clinical trials underway,” she said, “but right now, we don’t know the answer.”
More information
The National Psoriasis Foundation has more on psoriasis.
Copyright © 2026 HealthDay. All rights reserved.

